Shoulder
With the largest number of fellowship trained shoulder surgeons in the Mid-South region, OrthoSouth’s broad shoulder capabilities are represented at all of our Mid-South clinic locations.
Common Shoulder Injuries
The shoulder is a complex joint made up of three distinct bones and various soft tissues. Injuries to these structures are common and impact millions annually, from Memphis to the greater Mid-South and beyond. At OrthoSouth, our orthopedic physicians offer expert healing and compassionate care for a wide range of shoulder injuries and conditions. If you've been referred to a specialist for a shoulder injury, trust our doctors to provide the care you need and get you back to what matters.

Rotator Cuff Tears
Rotator Cuff Tears
Pain in the shoulder that caused limited range of motion and weakness
Rotator Cuff Tears

Shoulder Arthritis
Shoulder Arthritis
Pain, limited range of motion or a "catching" sensation in the shoulder that gets worse over time
Shoulder Arthritis
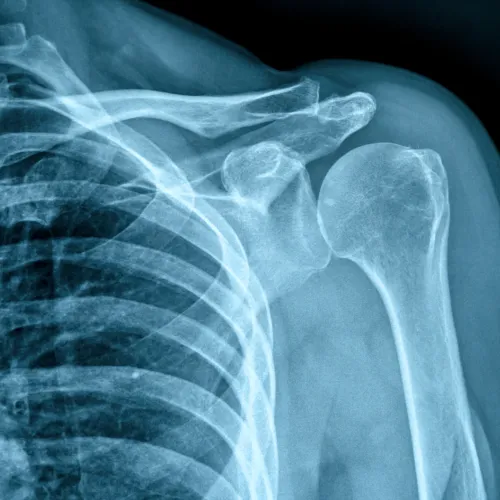
Shoulder Fractures
Shoulder Fractures
Broken clavicle, humerus or scapula
Shoulder Fractures

Shoulder Instability
Shoulder Instability
Also called shoulder dislocation or subluxation
Shoulder Instability
The following experienced and skilled OrthoSouth® surgeons are available to diagnose and treat your shoulder pain:
To view additional board-certified orthopedic physicians who are qualified to handle a range of shoulder issues, visit our provider page.