Total Joint Replacement
OrthoSouth's joint replacement surgeons offer unsurpassed personalized care and a full range of options customized to your needs and preferences, from same day outpatient knee replacement or hip replacement in one of our two convenient surgery centers, to MAKO Robotic Arm Assisted joint replacement surgery at nearby St. Francis Hospital and everything in between.
The following experienced and skilled OrthoSouth surgeons are available to evaluate your condition and perform your joint replacement surgery:
To view additional board-certified orthopedic physicians who are qualified to handle a range of joint-related issues, visit our provider page.
Learn More About Types of Joint Replacement
Total Hip Arthroplasty (Total Hip Replacement)
Total hip arthroplasty (also known as total hip replacement) has become one of the most common procedures performed. The specialists at OrthoSouth can safely and effectively perform a hip replacement to help restore you back to function.
Causes/Reasons
The procedure is mostly performed for hip osteoarthritis. Osteoarthritis is age and activity related wear and tear of the cartilage between the head of the femur (ball of the hip bone) and the acetabulum (socket). Normally, those two surfaces glide perfectly against each other as we walk, but with wear and tear of the cartilage, walking and activity can become painful and limiting.
Patients with hip arthritis can have symptoms like pain in the groin, pain when walking long distances, and even pain in the hip when putting on socks and shoes, or when getting into cars. Other reasons for hip replacement would be avascular necrosis, which is a disease of the head of the femur (ball of the hip bone) that causes the bone underneath the cartilage to weaken due to lack of blood flow. This lack of blood flow can be from various reasons, like a previous hip injury, chemotherapy or other drugs, sickle cell disease; or it can just happen for reasons not fully understood yet. An MRI is necessary to diagnose avascular necrosis. There are other reasons for a hip replacement as well, such as failed fixation after hip fractures, hip infections, and fractures of the neck of the femur (the part of the hip bone that connects the ball to the shaft).
The Procedure
In a total hip replacement, a surgical incision (cut) is made over the side of the hip and the neck of the femur is cut. The diseased hip ball is removed and a metal socket with plastic liner is placed in the socket. The femur bone is prepared for a stem, and connecting to the stem is a new metal ball. These pieces come in various sizes to fit your individual anatomy. The ball is placed in the socket and the incision is closed. After a hip replacement, the arthritis is gone and can't come back! Most people return to work, activities, and driving within a few weeks. Most patients go home the day after surgery, however select patients can go home on the same day after surgery.
There are various ways (approaches) to get to the hip with surgery. The two most common ways are the direct anterior approach and the posterolateral approach. Please ask your doctor for an explanation of each, but there are doctors at OrthoSouth that can perform one or either of these approaches.
Anterior Approach Hip Arthroplasty
With anterior approach hip arthroplasty there is no detachment or cutting of the muscles around the hip during surgery. This can result in more normal hip mechanics after surgery, allowing a more normal gait and less need for pain medications, with quicker return to function and a lower risk of hip dislocation.
Post-Surgery Physical Therapy
Physical therapy is needed after hip replacement to ensure continued muscle strength and a good outcome. The physical therapists at OrthoSouth are specially trained to get you strong and functional!
Total Knee Arthroplasty (Total Knee Replacement)
The goal of total or partial knee arthroplasty is to reduce pain and restore function and alignment in the knee.
What is arthritis?
The ends of our bones are coated with a substance called cartilage. Over time, due to a combination of age and genetics, this cartilage tends to erode leaving places of uncovered bone. This is what arthritis is - a loss of the cartilage cushioning and coating between bones that leads to arthritis.
Signs and Symptoms
- Stiffness, especially when you have been immobile for a period of time
- Pain associated with activity
- Loss of motion
- A sense of instability to the joint
Treatment Options
Non-Surgical Treatment
There are several non-operative treatments available to treat the symptoms of arthritis. Unfortunately there is no cure.
Anti-inflammatories (e.g. Advil, Meloxicam) are a good choice for flare ups. It is not recommended long term due to effects on the kidneys and liver.
Cortisone Injections are an option that can be administered every 3-4 months as needed for symptoms. These decrease the inflammatory response within the joint to decrease symptoms. If you are diabetic, they may temporarily raise your blood sugar levels.
Hyaluronic acid injections (e.g. Orthovisc, Euflexxa) act to improve the quality of the synovial fluid within the joint. Synovial fluid is a substance naturally found in the joint that provides lubrication. The injections do not regrow cartilage.
Surgical Treatment
When non-operative treatment does not provide symptom relief, you may consider a total or partial knee arthroplasty. A total knee arthroplasty is similar to retreading a tire. Small bone cuts are made to replace the articular surfaces of the joint with metal. A plastic spacer is inserted between the bones to act as a cushion.
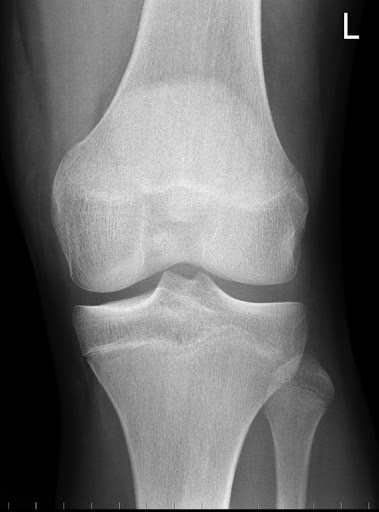
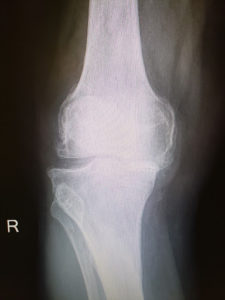
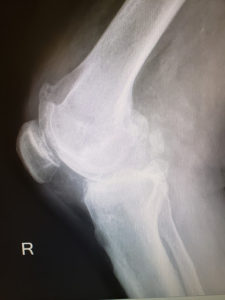
BEFORE SURGERY
In the first image you can see that the tibia and femur are touching and that there is bone to bone contact with bowing of the knee. The second image shows again bone to bone contact between the femur and tibia. The third image reveals arthritic changes between the patella and femur.
AFTER SURGERY
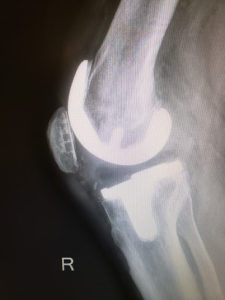
In the first image you can see the femur has been resurfaced and a cap has been placed on the end which is also visible in the 2nd picture. The tibia has a plate placed upon the end of it. The empty space between the bones represents a plastic space between the bones. The last picture shows the patella which has been resurfaced and retained with a small plastic button on the back.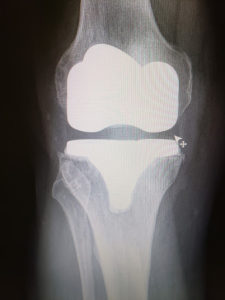
What Should I Expect with Surgery?
- Traditionally you are in the hospital for 1-2 days, but there is now a focus on same day surgery. This is an option to discuss with your provider.
- At the time of surgery, a combination of nerve blocks and both narcotic and non-narcotic pain medicines will be used which help with the amount of pain you have post-operatively.
- You will also be on medications to prevent blood clots following surgery.
- Recovery time is usually around 3 months. You should plan to be off work for 6 weeks to 3 months.
- It takes a full year for the knee to completely heal.
- At the end of the journey you will have a knee that no longer causes pain and should be able to do more of the things you enjoy.
Unicompartmental Knee Replacement (Partial Knee Replacement)
What is a unicompartmental (partial) knee replacement?
There are three "compartments" of the knee joint: medial (inside), lateral (outside), and patellofemoral (joint between the kneecap and the thighbone). The most common kind of knee replacement is a "total knee", in which all three compartments are resurfaced. Some people have knee arthritis that is isolated to one compartment (usually the medial). In a "Uni" or partial knee replacement, only the damaged portion of the knee is resurfaced, and the remainder of the knee is left intact.
Who is a candidate for a "Uni"?
The best candidate for a "uni" knee has pain only on one side of the knee, and mainly has pain just with weight bearing (not at rest). The X-ray should confirm that the arthritis is confined to one part of the knee. In addition, patients with unstable knees due to absent or non-functioning ligaments (the ACL, for instance), and those with inflammatory arthritis (rheumatoid, lupus, psoriasis, etc) are not candidates for unicompartmental replacement. In general, about 30% of patients with knee arthritis are candidates for the "uni".
What are the differences in a "uni" and a "total" knee?
The most important thing to remember is that both types of knee replacement work very well. There are several areas where unis differ from total knees.
In Unicompartmental knees, usually:
- The incision is smaller.
- There is less blood loss. Less than 1% of partial knee replacements require a blood transfusion.
- Risk of infection is lower.
- Stiffness is very uncommon and the ability to flex the knee is usually a little greater.
- Early recovery is faster. Most patients can go home on the day they have surgery. Patients get off their walker faster (usually 7-10 days) and physical therapy is not usually needed. By one year, function is about the same with partial and total knee replacement.
- Less bone is removed, so the knee feels a little more normal. It is generally easier to squat, kneel and use stairs with a unicompartmental compared to a total knee replacement. Most patients with a "uni" on one side and a "total" on the other prefer the "uni" knee.
- Revision is much easier. Because the "uni" surgery removes less bone and retains more of the native knee, if the implant fails, it is simpler to "re-do" or revise. Revision of a total knee replacement, while usually successful, has many potential pitfalls and the results are usually not as good as those of a primary total knee replacement. Results of revision of unicompartmental knee replacement to total knees are similar to those of primary or first time, total knee replacements.
The downside to unicompartmental knee replacement:
If unicompartmental knee replacement didn't have some drawbacks, everyone would do them. While the long-term results of uni knees are almost as good as those of total knees, they are not equal. Unicompartmental knees have a slightly higher failure rate than total knees. In the first year, about 3% of uni knees will fail because of implant loosening (compared to 1% of total knees). As time goes on, the native cartilage left behind can wear out, requiring revision to a total knee. As with a total knee, the implant is made of metal and plastic, and it can wear out also. Unicompartmental knees are also much more operator dependent. While total knees are done using a variety of cutting guides, uni knees are usually done "free hand", which requires the surgeon to make accurate cuts for optimal implant placement. In addition, not all knees are clear cut. While some knees clearly have arthritis involving only one compartment, many knees have advanced arthritis in one area, and mild arthritis in others. These knees require the surgeon to make a judgment call on whether a "Uni" is the appropriate implant. Factors such as patient age, size, and activity level also play a role. For these reasons, many surgeons choose not to do unicompartmental knee replacement and do exclusively total knee replacement.
What if the "uni" fails?
Depending on the reason for failure, the unicompartmental knee replacement can be revised to another "uni" or to a total knee. Because the "uni" removes so little bone, revising it to a total knee is similar to a primary, or first time, knee replacement.
Mako Robotic Arm Assisted Joint Replacement
Mako Robotic-Arm Assisted Knee and Hip Replacement Surgery
Mako Robotic-Arm Assisted Surgery is a minimally-invasive joint replacement surgery technique performed using an advanced, surgeon-controlled robotic arm system. Utilizing the system, your surgeon develops a customized surgery plan that uses a CT scan of your anatomy to optimize positioning of the implant. During the surgery, your surgeon uses feedback from the robotic arm to make real-time adjustments that some surgeons believe results in better accuracy for placement of the implant.
Dr. Jean Simard performs Mako Robotic Arm joint replacement surgeries at St. Francis Hospital in East Memphis.
CORI Robotic Assisted Outpatient Knee Replacement
Several OrthoSouth knee experts offer patients the option to combine the benefits of robot-assisted knee replacement with the experience of same day knee replacement at our Germantown Surgery Center.
Additional Information
Learn more by visiting the American Association of Orthopaedic Surgeons website on total joint replacement.