Hand & Wrist
The OrthoSouth Hand Center is comprised of fellowship-trained and board-certified orthopedic hand specialists, advanced practice professionals, and Certified Hand Therapists who are all focused on delivering the best patient experience in hand and wrist care available in the Mid-South (and beyond).
Hand & Wrist
The OrthoSouth Hand Center has a
4.86 out of 5 based on 1614 ratings on Google.
OrthoSouth takes a team approach to hand treatment, combining the expertise of hand and wrist surgeons and certified hand therapists. Our hand specialists have more than 60 years of collective clinical experience treating problems of the hand and wrist including carpal tunnel syndrome, trigger finger, tendinitis, arthritis, fractures, nerve compression, peripheral nerve damage, athletic injuries, trauma, and elective surgeries. Many of these issues can be treated with minimally invasive procedures by our expert surgeons, and in some cases with low-risk alternatives to traditional anesthesia.
All the members of the OrthoSouth hand and wrist surgery team are specially trained, experienced, and skilled in hand and wrist diagnoses, treatment and surgery. In addition to their extensive residency training, each orthopedic hand specialist has undergone advanced sub-specialty training and acquisition of skills in programs known as fellowships. These qualified hand and wrist surgeons provide each patient with superior knowledge and expertise in the area of hand surgery.
The following experienced and skilled OrthoSouth® surgeons have a combined Google rating of 4.86 out of 5 based on 1614 ratings:
Common Hand & Wrist Conditions
OrthoSouth® takes a team approach to hand treatment, combining the expertise of hand and wrist surgeons and certified hand therapists. Our hand specialists have more than 60 years of collective clinical experience treating problems of the hand and wrist including carpal tunnel syndrome, trigger finger, tendinitis, arthritis, fractures, nerve compression, peripheral nerve damage, athletic injuries, trauma, and elective surgeries. Many of these issues can be treated with minimally invasive procedures by our expert surgeons, and in some cases with low-risk alternatives to traditional anesthesia.
All the members of the OrthoSouth® hand and wrist surgery team are specially trained, experienced, and skilled in hand and wrist diagnoses, treatment and surgery. In addition to their extensive residency training, each orthopedic hand specialist has undergone advanced sub-specialty training and acquisition of skills in programs known as fellowships. These qualified hand and wrist surgeons provide each patient with superior knowledge and expertise in the area of hand surgery.

Carpal Tunnel Syndrome
Carpal Tunnel Syndrome
Pain and tingling in the wrist, forearm and hands.
Carpal Tunnel Syndrome
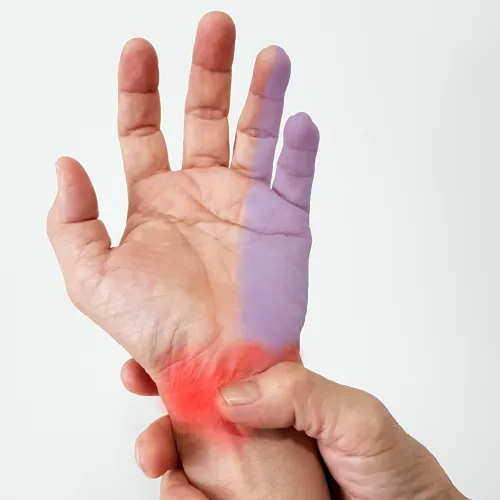
Ulnar Nerve Compression
Ulnar Nerve Compression
Fractures, arthritis, cysts and trauma can all cause nerve compression.
Ulnar Nerve Compression at Wrist

Trigger Finger/Thumb
Trigger Finger/Thumb
Catching, snapping or locking of a finger joint
Trigger Finger/Thumb

Wrist Fractures
Wrist Fractures
Breaks to the ulna, radius or some hand bones.
Wrist Fractures
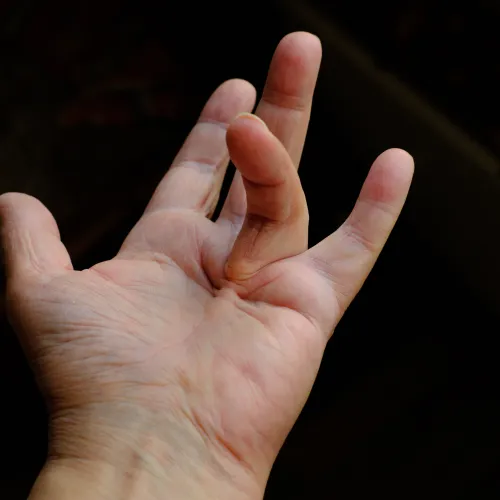
Dupuytren's Contracture
Dupuytren's Contracture
Pitting, bumps and cords in the hands that cause the fingers to bend into the palm.
Dupuytren's Contracture

Ganglion Cyst
Ganglion Cyst
Bumps in the wrist or around the base the finger that are tender to applied pressure
Ganglion Cyst
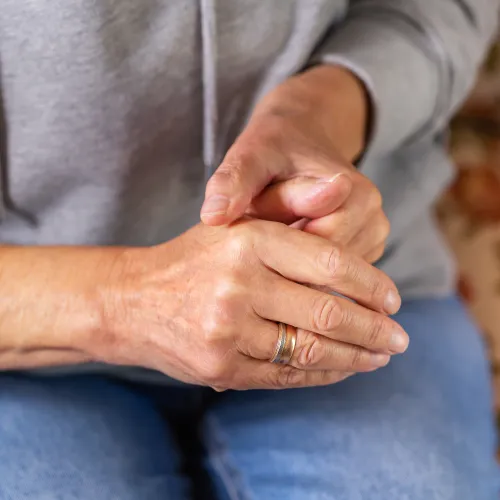
Thumb Arthritis
Thumb Arthritis
Pain and tenderness at the base of the thumb
Thumb Arthritis

Brachial Plexus Injury
Brachial Plexus Injury
A nerve injury that affects the muscles of the neck, shoulder, elbow wrist or hand.
Brachial Plexus Injury

Nerve Injury
Nerve Injury
Intermittent numbness, weakness or pain in the wrist or hand
Nerve Injury
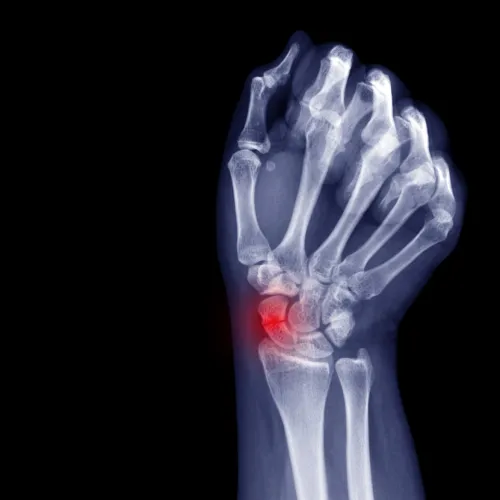
Scaphoid Fracture
Scaphoid Fracture
A break in the scaphoid bone in the wrist.
Scaphoid Fracture